The Smart Woman’s Guide To Heart Health
The Smart Woman’s Guide to Heart Health: Myths, Menopause & What Really Matters
When women think about health risks, breast cancer often comes top of mind.
But statistically?
Cardiovascular disease remains one of the leading causes of death in women.
Not to alarm you.
To empower you.
Because heart disease in women is often misunderstood, under-diagnosed, and influenced by factors that go far beyond weight or exercise alone.
So let’s break down the myths — and then I’ll show you what supports long-term heart health.
The Biggest Myths About Women’s Heart Health
#1 “Heart disease is a man’s problem.”
It really isn’t.
Heart disease is one of the leading causes of death in women. Yet women continue to be:
-
Under-represented in research into heart health
-
More likely to be underdiagnosed
-
More likely to experience symptoms that don’t look like the classic “Hollywood heart attack”
Women’s symptoms are typically more subtle:
-
Fatigue
-
Nausea
-
Jaw or back pain
-
Breathlessness
The heart is the same organ — but the presentation is definitely not.
#2 “If I’m slim, my heart must be healthy.”
Not necessarily.
You can be a completely “normal” weight and still have:
-
Visceral fat (that is the stuff padded around the organs and links to increased risk of chronic disease)
-
Insulin resistance
-
High LDL cholesterol (I've written a blog all about cholesterol here)
-
Chronic inflammation
Weight alone does not equal metabolic health.
This is particularly important for women in their 40s and 50s, when hormonal changes start to shift fat distribution and cholesterol patterns.
#3 “No family history of heart disease means I’m safe.”
Genetics matter — but they are not the full story.

Lifestyle, stress levels, sleep quality, hormonal shifts, blood pressure and metabolic health all significantly influence cardiovascular risk regardless of if there is a family history.
In many cases, lifestyle factors can either "turn on or turn off" a genetic predisposition.
#4 “I exercise regularly, so I should be fine.”
Don't get me wrong....exercise is incredibly protective..BUT....it cannot completely cancel out lifestyle factors such as:
-
Chronic stress
-
Poor sleep
-
High intake of ultra-processed foods
-
Smoking
-
High blood pressure
I heard a saying once that said - exercise is a good physical stress but not a cure for emotional stress. That really is so very true!
Same Heart — Different Risks
Men and women experience cardiovascular disease differently.
Hormones play a major role, especially during perimenopause and menopause.
Here's an infographic I have created that shows some of the key differences between men and women's hearts
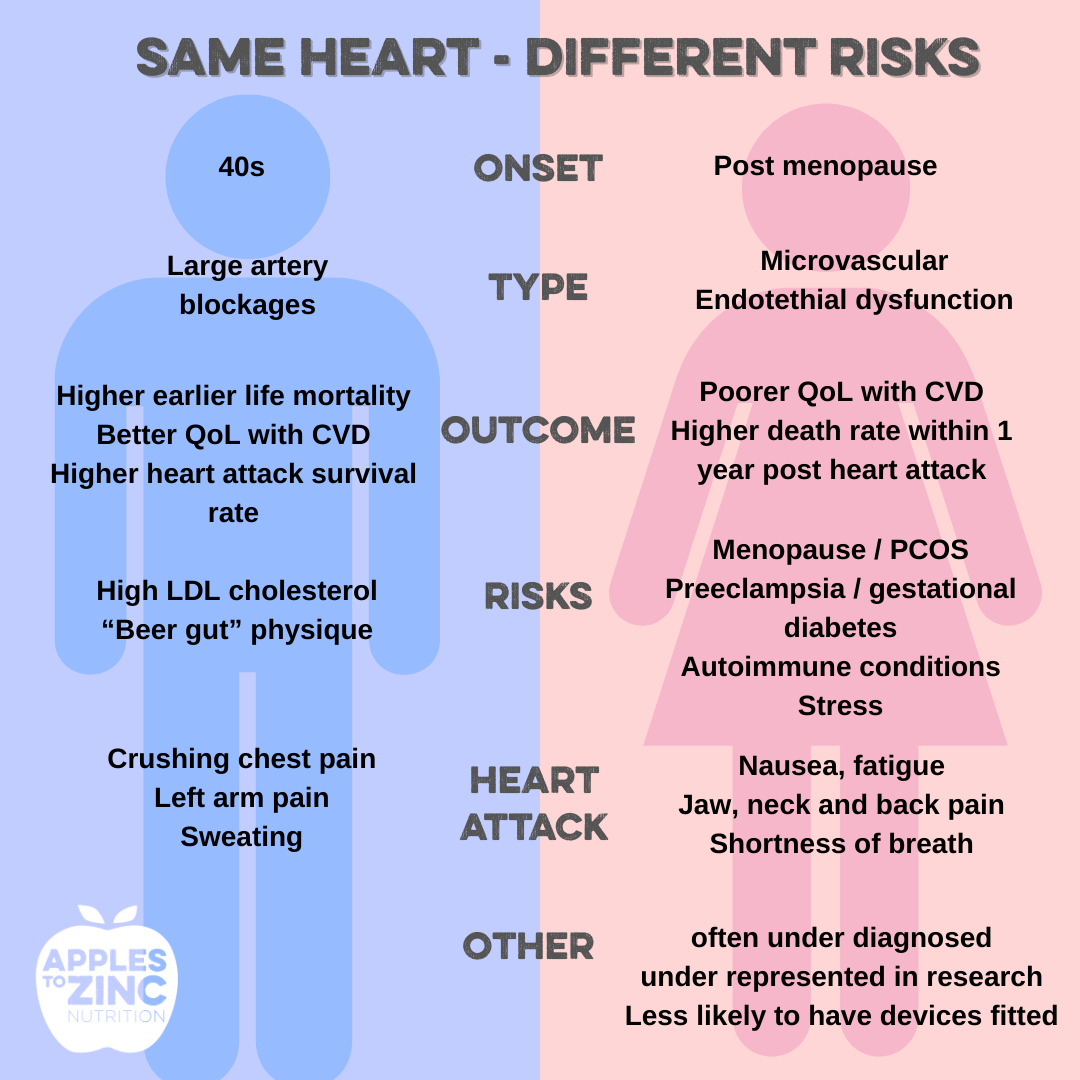
What Changes After Menopause?
 One of the biggest shifts is the decline in oestrogen.
One of the biggest shifts is the decline in oestrogen.
Oestrogen has a protective effect on the cardiovascular system. It helps:
-
Keep blood vessels flexible
-
Support healthy cholesterol balance
-
Improve insulin sensitivity
-
Reduce low-grade inflammation
As levels fluctuate and fall:
-
LDL (“bad”) cholesterol often rises
-
HDL (“good”) cholesterol may fall
-
Blood vessels can stiffen
-
Blood pressure may increase
-
Fat storage shifts towards the abdomen and the waist starts to thicken.
Importantly, these changes can happen even if your weight and diet haven’t changed.
This is why many women feel blindsided by “suddenly higher cholesterol.”
Research consistently shows cardiovascular risk accelerates after menopause — not simply because of age, but because of hormonal shifts.
Lifestyle Factors You May Be Overlooking
These are the quiet drivers of heart risk I see most often in clinic:
Chronic Stress

Elevated cortisol can drive:
-
Higher blood pressure readings
-
Inflammation
Poor Sleep
Sleep deprivation:
-
Impairs insulin sensitivity
-
Increases appetite hormones
-
Raises cardiovascular risk markers
Under Eating Protein
This contributes to:
-
Muscle loss
-
Reduced glucose control
-
Slower metabolism
Sedentary Work Days
 Prolonged sitting:
Prolonged sitting:
-
Reduces vascular flexibility
-
Lowers HDL cholesterol
Consuming Ultra-processed foods
These foods are typically higher in refined carbohydrates and sodium, low in fibre and phytonutrients and therefore are associated with increased cardiovascular risk
Your Heart Health Foundations: Work On What You Can Control
Rather than defaulting to “just eat less fat,” focus on what actually supports heart health.
💗 Maximise fibre (FREE FIBRE GUIDE)
Aim for 25–30g daily. Split this into 10g per meal to make it easier to achieve.
Fibre comes from foods such as:
-
Beans
-
Lentils
-
Vegetables
-
Fruits
-
Whole grains
💗 Prioritise omega-3 fats
Opt for oily fish twice weekly:
-
Salmon
-
Sardines
-
Mackerel
-
Fresh tuna
💗 Choose unsaturated fats
Use cold pressed extra virgin olive oil instead of butter, ghee or palm oils.
💗 Eat adequate protein (FREE PROTEIN GUIDE)
Around 1g per kg of ideal body weight to protect muscle and metabolic health.
💗 Include polyphenol-rich foods daily
These are in foods such as colourful berries, greens, teas, raw cacao.
💗 Eat potassium-rich foods
Vegetables, beans, fruit (especially bananas) to support healthy blood pressure.
💗 Train smart
Cardio supports heart health.
Strength training protects metabolism, mobility and independence.
I love this quote: “Cardio keeps you alive. Strength keeps you independent.”
What to Keep an Eye On
Here's a few of the markers (that aren't linked to the number on your scales!) to monitor. There are likely to help give you a sense of how much support your heart health needs.
-
Waist-to-height ratio (aim for waist less than half your height)
-
Fasting insulin
-
Triglycerides
-
Cholesterol ratios
-
Blood pressure trends
-
Stress levels
-
Sleep quality
